- Thyroid
- Beyond Acute COVID-19: Investigating the Incidence of Subacute Thyroiditis in Long COVID-19 in Korea
-
Jeongmin Lee, Gi Hyeon Seo, Keeho Song
-
Endocrinol Metab. 2023;38(4):455-461. Published online August 8, 2023
-
DOI: https://doi.org/10.3803/EnM.2023.1711
-
-
2,689
View
-
182
Download
-
3
Web of Science
-
4
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
The correlation between acute coronavirus disease 2019 (COVID-19) and subacute thyroiditis (SAT) has not been clearly investigated in “long COVID” patients. We aimed to investigate the incidence of SAT during convalescence and after the acute phase of COVID-19, comparing with that of the general population.
Methods
Data from a total of 422,779 COVID-19 patients and a control group of 2,113,895 individuals were analyzed. The index date was defined as the date 3 months after confirmation of COVID-19. The incidence rate (IR) of SAT and hazard ratios (HRs) were calculated per 100,000 persons. Subgroup analysis included analysis of HRs 90–179 and 180 days post-COVID-19 diagnosis; and additional analysis was conducted according to hospitalization status, sex, and age group.
Results
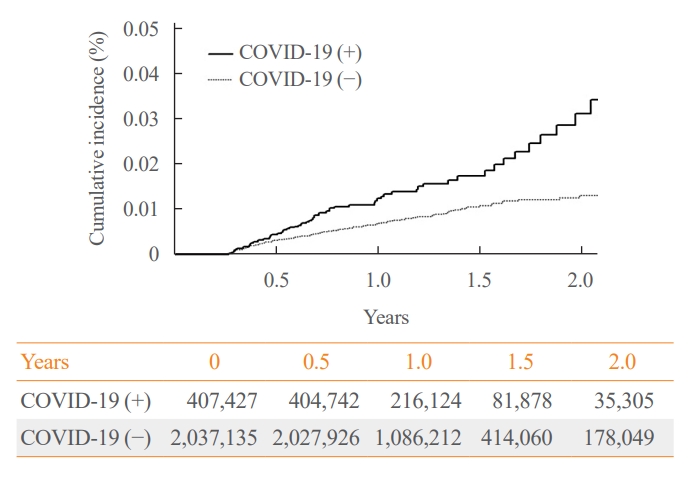
The IR of SAT was 17.28 per 100,000 persons (95% confidence interval [CI], 12.56 to 23.20) in the COVID-19 group and 8.63 (95% CI, 6.37 to 11.45) in the control group. The HR of COVID-19 patients was 1.76 (95% CI, 1.01 to 3.06; P=0.045). The HR of SAT was 1.39 (95% CI, 0.82 to 2.34; P=0.220) up to 6 months after the index date and 2.30 (95% CI, 1.60 to 3.30; P<0.001) beyond 6 months. The HR for SAT among COVID-19 patients was 2.00 (95% CI, 1.41 to 2.83) in hospitalized patients and 1.76 (95% CI, 1.01 to 3.06) in non-hospitalized patients compared to the control group. The IR of SAT was 27.09 (95% CI, 20.04 to 35.82) for females and 6.47 (95% CI, 3.34 to 11.30) for males. In the 19 to 64 age group, the IR of SAT was 18.19 (95% CI, 13.70 to 23.67), while the IR was 9.18 (95% CI, 7.72 to 10.84) in the 65 to 69 age group.
Conclusion
SAT could be a potential long-term complication of COVID-19. Long-term surveillance for thyroid dysfunction is needed especially in hospitalized, female and young-aged subjects.
-
Citations
Citations to this article as recorded by  - Thyroid dysfunction in COVID-19
David Tak Wai Lui, Chi Ho Lee, Yu Cho Woo, Ivan Fan Ngai Hung, Karen Siu Ling Lam
Nature Reviews Endocrinology.2024;[Epub] CrossRef - Subacute Thyroiditis in the Time of COVID-19
Hwa Young Ahn
Endocrinology and Metabolism.2024; 39(1): 186. CrossRef - Occult endocrine disorders newly diagnosed in patients with post-COVID-19 symptoms
Yasuhiro Nakano, Naruhiko Sunada, Kazuki Tokumasu, Hiroyuki Honda, Yuki Otsuka, Yasue Sakurada, Yui Matsuda, Toru Hasegawa, Daisuke Omura, Kanako Ochi, Miho Yasuda, Hideharu Hagiya, Keigo Ueda, Fumio Otsuka
Scientific Reports.2024;[Epub] CrossRef - rRisk of incident thyroid dysfunction in the post-acute phase of COVID-19: a population-based cohort study in Hong Kong
David Tak Wai Lui, Xi Xiong, Ching‐Lung Cheung, Francisco Tsz Tsun Lai, Xue Li, Eric Yuk Fai Wan, Celine Sze Ling Chui, Esther Wai Yin Chan, Franco Wing Tak Cheng, Lanlan Li, Matthew Shing Hin Chung, Chi Ho Lee, Yu Cho Woo, Kathryn Choon Beng Tan, Carlos
Endocrine Practice.2024;[Epub] CrossRef
- Adrenal gland
Big Data Articles (National Health Insurance Service Database)
- Mortality and Severity of Coronavirus Disease 2019 in Patients with Long-Term Glucocorticoid Therapy: A Korean Nationwide Cohort Study
-
Eu Jeong Ku, Keeho Song, Kyoung Min Kim, Gi Hyeon Seo, Soon Jib Yoo
-
Endocrinol Metab. 2023;38(2):253-259. Published online March 21, 2023
-
DOI: https://doi.org/10.3803/EnM.2022.1607
-
-
2,666
View
-
103
Download
-
2
Web of Science
-
2
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
The severity of coronavirus disease 2019 (COVID-19) among patients with long-term glucocorticoid treatment (LTGT) has not been established. We aimed to evaluate the association between LTGT and COVID-19 prognosis.
Methods
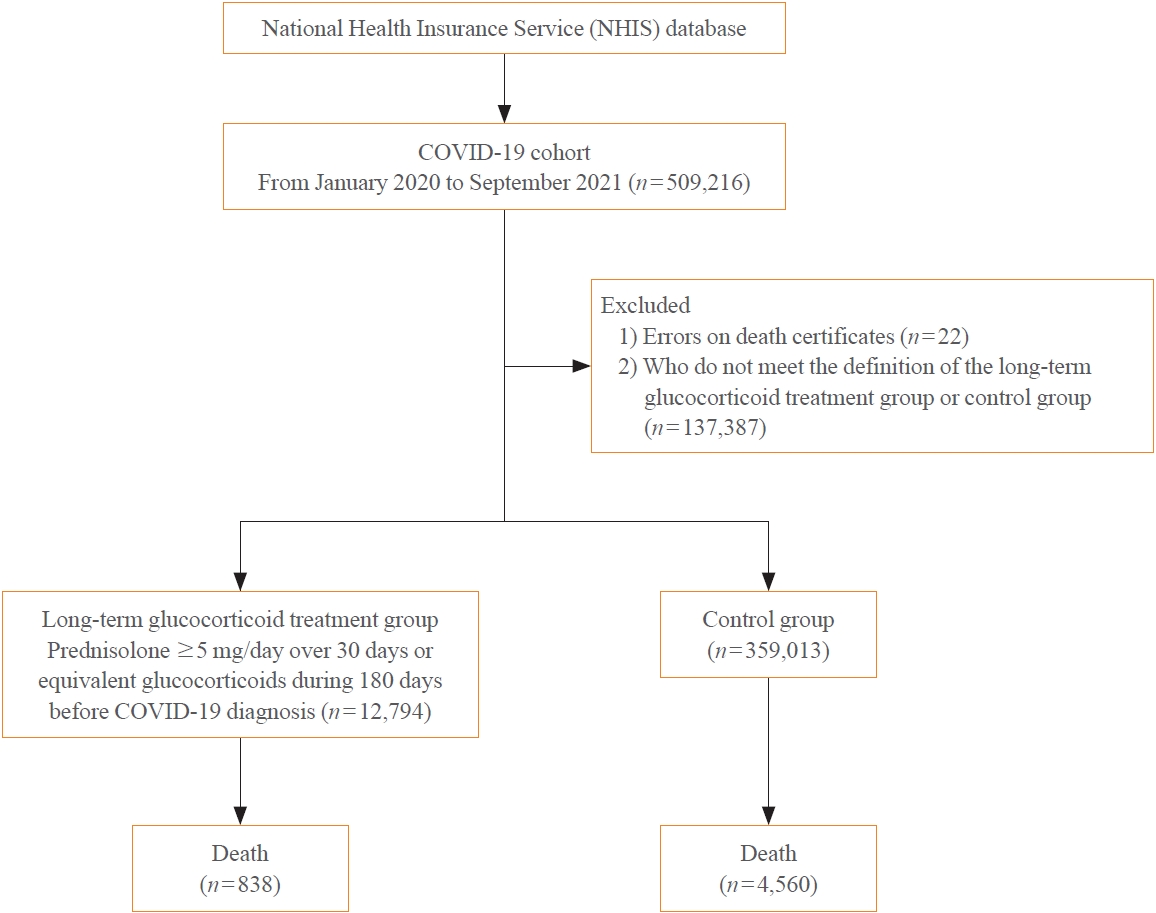
A Korean nationwide cohort database of COVID-19 patients between January 2019 and September 2021 was used. LTGT was defined as exposure to at least 150 mg of prednisolone (≥5 mg/day and ≥30 days) or equivalent glucocorticoids 180 days before COVID-19 infection. The outcome measurements were mortality, hospitalization, intensive care unit (ICU) admission, length of stay, and mechanical ventilation.
Results
Among confirmed patients with COVID-19, the LTGT group (n=12,794) was older and had a higher proportion of comorbidities than the control (n=359,013). The LTGT group showed higher in-hospital, 30-day, and 90-day mortality rates than the control (14.0% vs. 2.3%, 5.9% vs. 1.1%, and 9.9% vs. 1.8%, respectively; all P<0.001). Except for the hospitalization rate, the length of stay, ICU admission, and mechanical ventilation proportions were significantly higher in the LTGT group than in the control (all P<0.001). Overall mortality was higher in the LTGT group than in the control group, and the significance remained in the fully adjusted model (odds ratio [OR], 5.75; 95% confidence interval [CI], 5.31 to 6.23) (adjusted OR, 1.82; 95% CI, 1.67 to 2.00). The LTGT group showed a higher mortality rate than the control within the same comorbidity score category.
Conclusion
Long-term exposure to glucocorticoids increased the mortality and severity of COVID-19. Prevention and early proactive measures are inevitable in the high-risk LTGT group with many comorbidities.
-
Citations
Citations to this article as recorded by  - Glucocorticoids as a Double-Edged Sword in the Treatment of COVID-19: Mortality and Severity of COVID-19 in Patients Receiving Long-Term Glucocorticoid Therapy
Eun-Hee Cho
Endocrinology and Metabolism.2023; 38(2): 223. CrossRef - Pituitary Diseases and COVID-19 Outcomes in South Korea: A Nationwide Cohort Study
Jeonghoon Ha, Kyoung Min Kim, Dong-Jun Lim, Keeho Song, Gi Hyeon Seo
Journal of Clinical Medicine.2023; 12(14): 4799. CrossRef
- Diabetes, obesity and metabolism
Big Data Articles (National Health Insurance Service Database)
- Risk for Newly Diagnosed Type 2 Diabetes Mellitus after COVID-19 among Korean Adults: A Nationwide Matched Cohort Study
-
Jong Han Choi, Kyoung Min Kim, Keeho Song, Gi Hyeon Seo
-
Endocrinol Metab. 2023;38(2):245-252. Published online April 5, 2023
-
DOI: https://doi.org/10.3803/EnM.2023.1662
-
-
2,319
View
-
122
Download
-
2
Web of Science
-
2
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
Coronavirus disease 2019 (COVID-19) can cause various extrapulmonary sequelae, including diabetes. However, it is unclear whether these effects persist 30 days after diagnosis. Hence, we investigated the incidence of newly diagnosed type 2 diabetes mellitus (T2DM) in the post-acute phase of COVID-19.
Methods
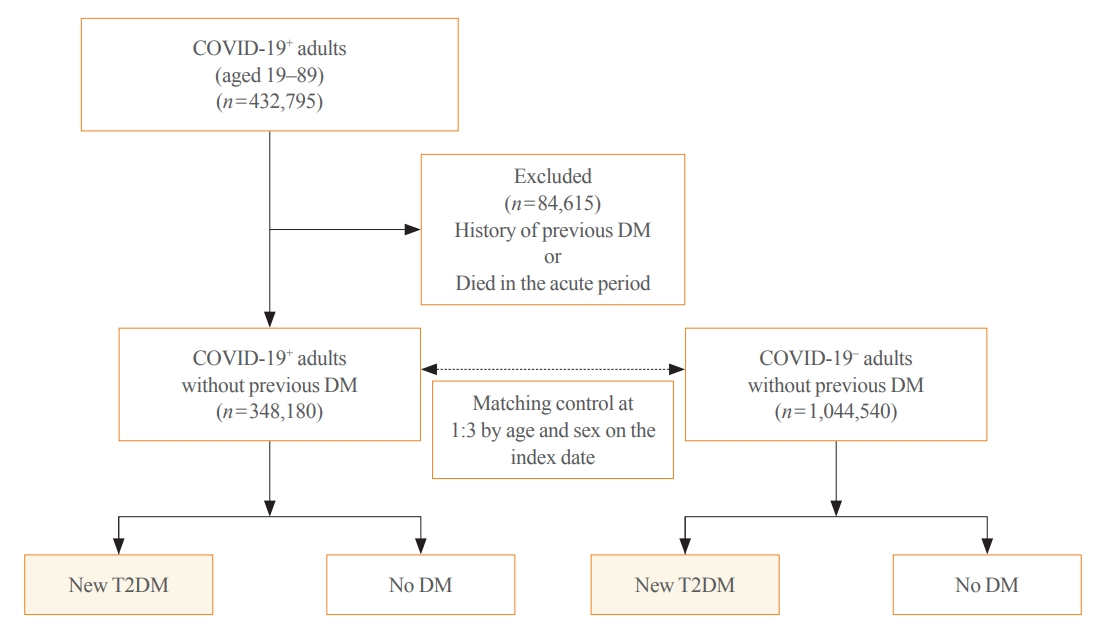
This cohort study used data from the Health Insurance Review and Assessment Service, a representative national healthcare database in Korea. We established a cohort of 348,180 individuals diagnosed with COVID-19 without a history of diabetes between January 2020 and September 2021. The control group consisted of sex- and age-matched individuals with neither a history of diabetes nor COVID-19. We assessed the hazard ratios (HR) of newly diagnosed T2DM patients with COVID-19 compared to controls, adjusted for age, sex, and the presence of hypertension and dyslipidemia.
Results
In the post-acute phase, patients with COVID-19 had an increased risk of newly diagnosed T2DM compared to those without COVID-19 (adjusted HR, 1.30; 95% confidence interval [CI], 1.27 to 1.33). The adjusted HRs of non-hospitalized, hospitalized, and intensive care unit-admitted patients were 1.14 (95% CI, 1.08 to 1.19), 1.34 (95% CI, 1.30 to 1.38), and 1.78 (95% CI, 1.59 to 1.99), respectively. The risk of T2DM in patients who were not administered glucocorticoids also increased (adjusted HR, 1.29; 95% CI, 1.25 to 1.32).
Conclusion
COVID-19 may increase the risk of developing T2DM beyond the acute period. The higher the severity of COVID-19 in the acute phase, the higher the risk of newly diagnosed T2DM. Therefore, T2DM should be included as a component of managing long-term COVID-19.
-
Citations
Citations to this article as recorded by  - New-Onset Diabetes Mellitus in COVID-19: A Scoping Review
Anca Pantea Stoian, Ioana-Cristina Bica, Teodor Salmen, Wael Al Mahmeed, Khalid Al-Rasadi, Kamila Al-Alawi, Maciej Banach, Yajnavalka Banerjee, Antonio Ceriello, Mustafa Cesur, Francesco Cosentino, Alberto Firenze, Massimo Galia, Su-Yen Goh, Andrej Janez,
Diabetes Therapy.2024; 15(1): 33. CrossRef - Pituitary Diseases and COVID-19 Outcomes in South Korea: A Nationwide Cohort Study
Jeonghoon Ha, Kyoung Min Kim, Dong-Jun Lim, Keeho Song, Gi Hyeon Seo
Journal of Clinical Medicine.2023; 12(14): 4799. CrossRef
- Thyroid
- Incidence and Prevalence of Overt Hypothyroidism and Causative Diseases in Korea as Determined Using Claims Data Provided by the Health Insurance Review and Assessment Service
-
Gi Hyeon Seo, Jae Hoon Chung
-
Endocrinol Metab. 2015;30(3):288-296. Published online January 5, 2015
-
DOI: https://doi.org/10.3803/EnM.2015.30.3.288
-
-
3,829
View
-
46
Download
-
15
Web of Science
-
15
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
The incidence and prevalence of overt hypothyroidism have been reported to be 2 to 4/1,000 population/year and 8 to 13/1,000 population, respectively, in foreign countries. As there has been no nationwide survey to obtain data in Korea, the present study investigated the incidence and prevalence of overt hypothyroidism in Korea using claims data provided by the Health Insurance Review and Assessment Service. The proportions of causative diseases for hypothyroidism were also analyzed. MethodsThis study was retrospectively performed with 541,969 Korean patients (92,832 men and 449,137 women), with overt hypothyroidism, treated with thyroid hormone between 2008 and 2012. ResultsThe incidence of overt hypothyroidism in Korea was 2.26/1,000 population/year (0.78 in men and 3.72 in women), and the prevalence was 14.28/1,000 population (4.40 in men and 24.03 in women). When patients with thyroid cancer were excluded, the incidence was 1.56/1,000 population/year (0.54 in men and 2.57 in women). The incidence increased with age, with peaks in and after the late 60s in men and in the early 50s in women. The prevalence peaked in the early 70s in men and in the late 50s in women. ConclusionThis is a report of the first nationwide investigation of the incidence and prevalence of overt hypothyroidism in Korea, although it is limited to patients treated with thyroid hormone.
-
Citations
Citations to this article as recorded by  - Association of Thyroid Hormone Medication Adherence With Risk of Dementia
Saemi Han, Seogsong Jeong, Seulggie Choi, Sun Jae Park, Kyae Hyung Kim, Gyeongsil Lee, Yoosun Cho, Joung Sik Son, Sang Min Park
The Journal of Clinical Endocrinology & Metabolism.2023; 109(1): e225. CrossRef - The impact of the micronutrient iodine in health and diseases
Ma. Cecilia Opazo, Irenice Coronado-Arrázola, Omar P. Vallejos, Rodrigo Moreno-Reyes, Carlos Fardella, Lorena Mosso, Alexis M. Kalergis, Susan M. Bueno, Claudia A. Riedel
Critical Reviews in Food Science and Nutrition.2022; 62(6): 1466. CrossRef - Hypothyroidism risk associated with rheumatoid arthritis
Chung-Ming Huang, Fung-Chang Sung, Hsuan-Ju Chen, Che-Chen Lin, Cheng-Li Lin, Po-Hao Huang
Medicine.2022; 101(1): e28487. CrossRef - Risk of All-Cause Mortality in Levothyroxine-Treated Hypothyroid Patients: A Nationwide Korean Cohort Study
Seo Young Sohn, Gi Hyeon Seo, Jae Hoon Chung
Frontiers in Endocrinology.2021;[Epub] CrossRef - Update on Thyroid Hormone Levels and Thyroid Dysfunction in the Korean Population Based on Data from the Korea National Health and Nutrition Examination Survey VI (2013 to 2015)
Jae Hoon Chung
Endocrinology and Metabolism.2020; 35(1): 7. CrossRef - Treatment of hypothyroidism using Korean medicine: 2 case reports
Hyongjun Kim, Sun-Young Moon, Kyungsun Han, Jun-Hwan Lee, Jong Hwan Im, Sungha Kim, Jeong-Eun Yoo
Medicine.2020; 99(18): e19737. CrossRef - Genotype association of IP6K3 gene with Hashimoto’s thyroiditis in Algerian population (Aures region)
Warda Kherrour, Dean Kalicanin, Luka Brčić, Leila Hambaba, Mouloud Yahia, Souheyla Benbia, Vesna Boraska Perica
Egyptian Journal of Medical Human Genetics.2020;[Epub] CrossRef - Prevalence of Thyroid Disease in Patients Surgically Treated for Pituitary Disease
Kim, Cho, Ku, Jung, Moon, Kim, Shin, Kim, Lee
Journal of Clinical Medicine.2019; 8(8): 1142. CrossRef - Medical Big Data Is Not Yet Available: Why We Need Realism Rather than Exaggeration
Hun-Sung Kim, Dai-Jin Kim, Kun-Ho Yoon
Endocrinology and Metabolism.2019; 34(4): 349. CrossRef - Evaluation of Thyroid Hormone Levels and Urinary Iodine Concentrations in Koreans Based on the Data from Korea National Health and Nutrition Examination Survey VI (2013 to 2015)
Jae Hoon Chung
Endocrinology and Metabolism.2018; 33(2): 160. CrossRef - Prevalence and Annual Incidence of Thyroid Disease in Korea from 2006 to 2015: A Nationwide Population-Based Cohort Study
Hyemi Kwon, Jin-hyung Jung, Kyung-Do Han, Yong-Gyu Park, Jung-Hwan Cho, Da Young Lee, Ji Min Han, Se Eun Park, Eun-Jung Rhee, Won-Young Lee
Endocrinology and Metabolism.2018; 33(2): 260. CrossRef - Thyroid Stimulating Hormone Reference Range and Prevalence of Thyroid Dysfunction in the Korean Population: Korea National Health and Nutrition Examination Survey 2013 to 2015
Won Gu Kim, Won Bae Kim, Gyeongji Woo, Hyejin Kim, Yumi Cho, Tae Yong Kim, Sun Wook Kim, Myung-Hee Shin, Jin Woo Park, Hai-Lin Park, Kyungwon Oh, Jae Hoon Chung
Endocrinology and Metabolism.2017; 32(1): 106. CrossRef - The relationship of 19 functional polymorphisms in iodothyronine deiodinase and psychological well-being in hypothyroid patients
Yoon Young Cho, Hye Jeong Kim, Hye Won Jang, Tae Hyuk Kim, Chang-Seok Ki, Sun Wook Kim, Jae Hoon Chung
Endocrine.2017; 57(1): 115. CrossRef - Concomitant Thyroid Disorders and Inflammatory Bowel Disease: A Literature Review
Toru Shizuma
BioMed Research International.2016; 2016: 1. CrossRef - Hypothyroidism among SLE patients: Case–control study
Abdulla Watad, Naim Mahroum, Aaron Whitby, Smadar Gertel, Doron Comaneshter, Arnon D. Cohen, Howard Amital
Autoimmunity Reviews.2016; 15(5): 484. CrossRef
|